Connect With Us

Special Needs Population and Custom Orthotics
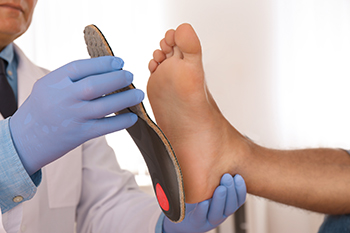
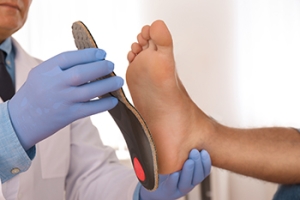
For individuals with special needs, foot and ankle conditions are often more prevalent, necessitating careful consideration when prescribing custom orthotics. Conditions like plantar fasciitis, medial tibial stress syndrome, hallux limitus, and rigidus are commonly observed, especially among those with Down syndrome or Fragile X syndrome. When designing orthotics for special needs patients, modifications may be required to accommodate unique foot shapes and biomechanical issues. Attention to materials and shoe compatibility is important to ensure optimal support and comfort. A biomechanical examination is essential to assess gait patterns and identify specific needs. Podiatrists specialize in working with such patients, providing tailored orthotic solutions, and collaborating with caregivers to address individual requirements effectively. If you have special needs and have foot issues, or if you are caring for such an individual, it is suggested that you schedule an appointment with a podiatrist who can help enhance their mobility, comfort, and overall foot health.
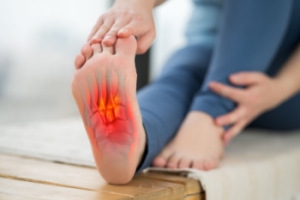
Discover relief from persistent foot pain with custom orthotics and shoe inserts. If you’re battling heel pain, these personalized solutions offer targeted support, addressing the root causes of discomfort. Customized to your unique biomechanics, these inserts provide stability, alleviating both heel and foot pain. Say goodbye to the agony of every step and hello to a life free from constant foot pain. Invest in your well-being with custom orthotics or shoe inserts ensuring your feet receive the care they deserve. Step confidently, step comfortably – because a pain-free journey begins with the right support.
If you have any questions please contact our office located in El Paso, TX . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Investing in Custom Orthotics Means Investing in Foot Health
Custom orthotics offer a tailored approach to foot health, providing a host of benefits that extend far beyond conventional shoe inserts. One of the primary advantages lies in their ability to address specific biomechanical issues. Unlike off-the-shelf inserts, custom orthotics are crafted based on an individual's unique foot structure, gait, and any existing foot conditions.
The personalized design of custom orthotics ensures optimal support for the arches, promoting proper alignment and distributing pressure evenly across the feet. This can be particularly beneficial for individuals dealing with issues such as overpronation or underpronation, as custom orthotics help correct imbalances that may lead to discomfort or injury.
Beyond biomechanics, custom orthotics can alleviate a range of foot problems, including plantar fasciitis, bunions, and metatarsalgia. They provide targeted relief to areas under stress, reducing pain and inflammation. Additionally, for those with specific medical conditions like diabetes, custom orthotics can play a crucial role in preventing complications associated with poor foot health.
Comfort is another key aspect of custom orthotics. By accommodating the unique contours of an individual's feet, these inserts enhance overall comfort, making daily activities more enjoyable. Whether for athletes looking to optimize performance or individuals seeking relief from chronic foot pain, custom orthotics offer a versatile solution.
Investing in custom orthotics is an investment in long-term foot health. They not only provide immediate relief but also contribute to the prevention of future issues. With the ability to seamlessly integrate into various types of footwear, custom orthotics empower individuals to prioritize foot comfort without compromising on style. In essence, custom orthotics are a personalized prescription for happy, healthy, and pain-free feet.
Causes and Symptoms of Lisfranc Fractures
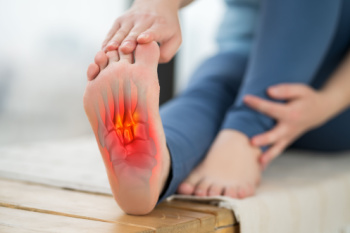
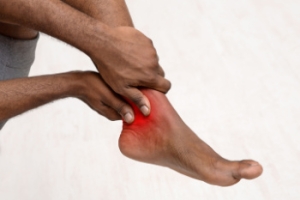
Lisfranc fractures or injuries, although rare, can be incredibly painful and often require prompt diagnosis and treatment. These injuries affect the joints in the middle of the foot, and while Lisfranc fractures can sometimes be mistaken for a sprain, they necessitate specialized care from a podiatrist. Causes include sports-related trauma, and everyday accidents like falling down stairs or having an object land on the foot. Among the symptoms are tenderness, swelling, bruising, and severe pain while standing or walking. Diagnosis typically involves a physical examination and X-rays, with further imaging like CT scans or MRIs sometimes necessary for surgical planning. In some cases, conservative treatment methods like immobilization with a cast or boot may suffice. In more severe cases, surgery may be prescribed, particularly if there are fractures, dislocations, or extensive soft tissue damage. If you are experiencing symptoms of a Lisfranc injury or have recently sustained an injury to your foot, it is suggested that you schedule an appointment with a podiatrist for an exam and treatment options.
A broken foot requires immediate medical attention and treatment. If you need your feet checked, contact David Williams, DPM from El Paso Feet. Our doctor can provide the care you need to keep you pain-free and on your feet.
Broken Foot Causes, Symptoms, and Treatment
A broken foot is caused by one of the bones in the foot typically breaking when bended, crushed, or stretched beyond its natural capabilities. Usually the location of the fracture indicates how the break occurred, whether it was through an object, fall, or any other type of injury.
Common Symptoms of Broken Feet:
- Bruising
- Pain
- Redness
- Swelling
- Blue in color
- Numbness
- Cold
- Misshapen
- Cuts
- Deformities
Those that suspect they have a broken foot shoot seek urgent medical attention where a medical professional could diagnose the severity.
Treatment for broken bones varies depending on the cause, severity and location. Some will require the use of splints, casts or crutches while others could even involve surgery to repair the broken bones. Personal care includes the use of ice and keeping the foot stabilized and elevated.
If you have any questions please feel free to contact our office located in El Paso, TX . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Causes, Symptoms, and Treatment for a Broken Foot
One out of ten broken bones is reported to be in the feet. When an object crushes, bends, or stretches the bone beyond acceptable ranges, bones break. A break in the foot is either a fracture or a straight break.
The location of any break can tell you how the break happened. Toes, for instance, break typically as a result of something being kicked hard and with great force. Heel breaks almost always are a result of an improper landing from a tall height. Twists or sprains are the other two frequent occurrences. As with all usual breaks, they result from unexpected accident or sudden injury. As with stress fractures, breaks form as a process over time from repeated stress on already present cracks. Runners, dancers, and gymnasts are the usual athletes who receive this type of break. Stress fractures result from incredible pressure on the feet. It is no surprise these athletes bear the majority of reported fractures.
Pain, swelling, bruising, and redness are all indicative of the typical symptoms from a broken foot. Severe pain—to the point of not being able to walk—usually depends on the location of the break in the foot. Toes are on the lower scale of pain threshold, but heels are high, as are a few other particular bones. As the severity of the broken foot increases, symptoms like blueness, numbness, misshaping of the foot, cuts, or deformities will become apparent. These symptoms indicate the need to see a medical professional with access to an x-ray facility.
Prior to seeing a specialist, precautions should be taken to reduce pain and swelling. Elevate and stabilize the foot, and refrain from moving it. Immobilization of the foot is the next priority, so creating a homemade splint is acceptable. Keep in mind that while creating a splint, any increase of pain or cutting off blood circulation means that the splint should be removed immediately. Use ice to decrease swelling and relieve pain symptoms.
When dealing with a medical center, the patient should note that the treatment can vary. The treatment will depend on the severity of the fracture and the cause of the break. Crutches, splits, or casts are common treatments while surgery has been known to be used in more severe cases in order to repair the break in the bones.
Early Indications of Rheumatoid Arthritis and Its Impact on the Feet

Rheumatoid arthritis, or RA, manifests through subtle yet telling signs, especially in its early stages. A common indicator is persistent joint stiffness, particularly in the mornings or after periods of inactivity. Accompanying this stiffness is often joint pain and swelling, which can gradually worsen over time. RA does not discriminate, affecting various joints throughout the body, including those in the feet. In fact, the feet are commonly among the first areas affected by RA. The condition can lead to inflammation in the joints of the feet, causing pain, swelling, and difficulty with mobility. Over time, RA may cause deformities such as bunions, hammertoes, or joint collapse in severe cases. If you are experiencing any of the above symptoms in your feet, it is strongly suggested that you are under the care of a podiatrist who can offer you effective management strategies.
Because RA affects more than just your joints, including the joints in your feet and ankles, it is important to seek early diagnosis from your podiatrist if you feel like the pain in your feet might be caused by RA. For more information, contact David Williams, DPM of El Paso Feet. Our doctor will assist you with all of your podiatric concerns.
What Is Rheumatoid Arthritis?
Rheumatoid Arthritis (RA) is an autoimmune disorder in which the body’s own immune system attacks the membranes surrounding the joints. Inflammation of the lining and eventually the destruction of the joint’s cartilage and bone occur, causing severe pain and immobility.
Rheumatoid Arthritis of the Feet
Although RA usually attacks multiple bones and joints throughout the entire body, almost 90 percent of cases result in pain in the foot or ankle area.
Symptoms
- Swelling and pain in the feet
- Stiffness in the feet
- Pain on the ball or sole of feet
- Joint shift and deformation
Diagnosis
Quick diagnosis of RA in the feet is important so that the podiatrist can treat the area effectively. Your doctor will ask you about your medical history, occupation, and lifestyle to determine the origin of the condition. Rheumatoid Factor tests help to determine if someone is affected by the disease.
If you have any questions please feel free to contact our office located in El Paso, TX . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Rheumatoid Arthritis in the Feet
Although rheumatoid arthritis attacks multiple bones and joints throughout the entire body, ninety percent of people who actually develop this condition usually do so in the foot or ankle area. Those who develop this kind of arthritis in the feet usually develop symptoms around the toes and forefeet first, before anywhere else. Rheumatoid arthritis appears to have a genetic component. If it runs in the family, then you will be more likely to develop it as well.
Rheumatoid arthritis is an autoimmune disorder in which the body’s own immune system attacks the lining of the membranes surrounding the joints. This causes inflammation of the membrane lining, and the gradual destruction of the joint’s cartilage and even bone.
Some of the most common symptoms that are associated with RA include pain and swelling of the feet. Stiffness in the feet is also another common symptom that people experience. Those who have RA in the feet usually feel the pain in the ball or sole of their feet. This can get to be very painful at times. A person's joints can even shift and become deformed after a period of time.
In order to properly diagnose RA in the feet it is usually necessary for a doctor or podiatrist to evaluate the area. Your doctor will also question you about your medical history, occupation, etc., to determine whether anything in your lifestyle may have triggered the condition. There are a number of tests that may be performed to help diagnose RA, such as a rheumatoid factor test. There is, however, no one single test that will tell you for sure if you have RA. There are different X-rays that can be taken as well to determine if a person has RA in their feet.
There is a range of treatment options for rheumatoid arthritis. Treatment of RA is usually a lifelong process that includes a variety of methods of treatment and therapy. Your doctor can prescribe special shoes that should help with arch support as well as heel support. A physical therapist can help those with this condition learn exercises which will keep their joints flexible. Surgery may be needed to correct some of the issues with the feet, such as bunions, and hammertoes. Fusion is usually the most successful surgical option for rheumatoid arthritis. However, people need to keep in mind that there are some risks associated with these surgeries.
Corns Caused by Friction
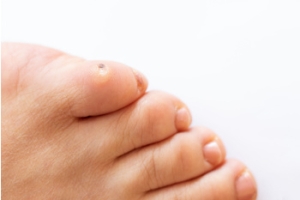
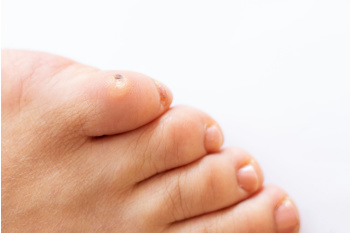 Corns on the feet are often the result of rubbing and mechanical stress on the skin. When there is repetitive friction on a certain area of the foot, the skin may respond by thickening and forming a hardened, raised bump known as a corn. Bony prominences, such as the toes or the sides of the feet, are more susceptible to corn development caused by rubbing against the shoes. Corns can also form in response to wearing ill-fitting footwear, high heels, or possibly from having foot deformities that alter the distribution of weight and pressure on the feet. While corns themselves are not usually harmful, they can cause discomfort or pain, especially when walking or wearing shoes. Podiatrists, or foot doctors, can address corns through various treatments, such as trimming, padding, or orthotic devices to provide relief. If you are struggling with corns on the feet, it is suggested that you consult a podiatrist for personalized treatment options.
Corns on the feet are often the result of rubbing and mechanical stress on the skin. When there is repetitive friction on a certain area of the foot, the skin may respond by thickening and forming a hardened, raised bump known as a corn. Bony prominences, such as the toes or the sides of the feet, are more susceptible to corn development caused by rubbing against the shoes. Corns can also form in response to wearing ill-fitting footwear, high heels, or possibly from having foot deformities that alter the distribution of weight and pressure on the feet. While corns themselves are not usually harmful, they can cause discomfort or pain, especially when walking or wearing shoes. Podiatrists, or foot doctors, can address corns through various treatments, such as trimming, padding, or orthotic devices to provide relief. If you are struggling with corns on the feet, it is suggested that you consult a podiatrist for personalized treatment options.
If you have any concerns regarding your feet and ankles, contact David Williams, DPM of El Paso Feet. Our doctor will treat your foot and ankle needs.
Corns: What Are They? and How Do You Get Rid of Them?
Corns can be described as areas of the skin that have thickened to the point of becoming painful or irritating. They are often layers and layers of the skin that have become dry and rough, and are normally smaller than calluses.
Ways to Prevent Corns
There are many ways to get rid of painful corns such as wearing:
- Well-fitting socks
- Comfortable shoes that are not tight around your foot
- Shoes that offer support
Treating Corns
Treatment of corns involves removing the dead skin that has built up in the specific area of the foot. Consult with Our doctor to determine the best treatment option for your case of corns.
If you have any questions please feel free to contact our office located in El Paso, TX . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Corns: What Are They, and How Do You Get Rid of Them
Corns are thickened areas on the skin’s surface, to the point of being irritating and sometimes painful. Commonly found on the feet, corns are circular or cone-shaped. They develop where there are areas of pressure or friction, such as on the little toe when it rubs up against shoes, or on the ball of your foot.
Corns are often confused with a callus, but there is a difference between them. Corns can be raised bumps that are painful to the touch. They consist of a rough, thick area of skin that may be dry or waxy. Corns tend to be surrounded by skin that is inflamed, and are usually much smaller than calluses.
Removing the dead skin that has built up is the key in treating corns. Salicylic acid medication is most common in accomplishing this. The acid works by dissolving keratin, which is the protein that makes up the majority of corns. You can purchase salicylic acid over-the-counter in products such as wart removers. It comes in a variety of forms such as medicated pads, drops, or creams. However, people who are diabetic should not use salicylic acid, but should instead consult their doctor immediately.
According to the product directions, applying the medication directly onto the corn will treat it. The top layer of the corn will begin to turn white after use. When that occurs, the layers of skin can then be peeled away, making the corn smaller. Shaving off corns with razors or other pedicure equipment is never a good idea. This can lead to infection. If your corn gets infected, and is not treated immediately, a visit to the doctor will be necessary.
Another way to treat corns and help prevent their return is by using orthotic inserts, fitted by a podiatrist. Inserts fit right into your shoes and adjusts the way your foot fits into your shoes. This fixes the way you walk. This will lower your chances of getting corns, and eliminate current corns by reducing rubbing from friction.
Surgery is rarely used to treat corns, but does occur on occasion. Surgery actually deals with the underlying issue that causes corns. During surgery, the bone is shaved and any abnormalities are corrected, thus reducing the amount of friction that occurs during walking.
To prevent corns, the first step is reducing friction. Always wear shoes that fit well and don’t rub your feet. Pads can be purchased if you notice rubbing developing. These pads can be purchased over-the-counter, and can be simply placed on the irritated area. Wearing cushioned insoles in your shoes can always reduce the friction, and making sure to wear well-fitting shoes. This will ensure that your foot is not being squeezed awkwardly, and prevent corns from forming in the first place.
Custom Orthotics Seasonal - Any Season

Rain or shine, snow or sleet, Custom Orthotics have your feet covered! As the seasons change, ensure your steps remain comfortable and supported. Custom Orthotics adapt to your footwear, from summer sandals to winter boots, providing consistent relief and alignment. Don't let the changing weather dictate your foot comfort. Step confidently year-round and experience the difference with Custom Orthotics. Call today for more information.